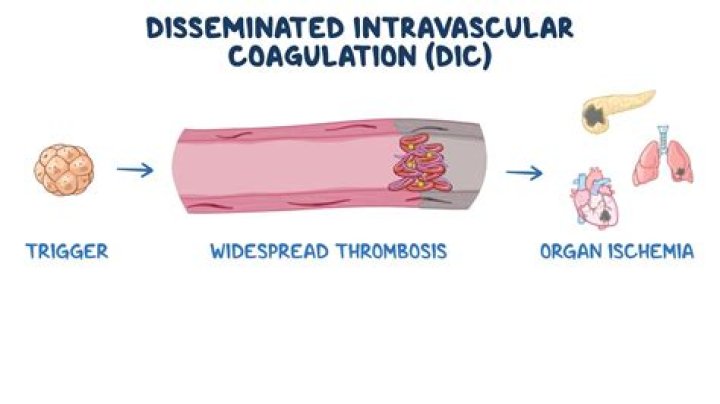
Clinical features: DIC may present as acute, subacute or chronic disease. Acute DIC may develop primarily (e.g. caused by sepsis), or secondary to decompensation of chronic DIC. Acute DIC is often fatal with multiorgan failure and circulatory collapse. Acute DIC is more commonly observed in dogs and is rare in cats.Similarly, it is asked, can you die from DIC?
Disseminated intravascular coagulation (DIC) is a rare, life-threatening condition. In the early stages of the condition, DIC causes your blood to clot excessively. As a result, blood clots may reduce blood flow and block blood from reaching bodily organs. DIC is a serious condition that can lead to death.
Subsequently, question is, what is the survival rate of DIC? Prognosis varies depending on the underlying disorder, and the extent of the intravascular thrombosis (clotting). The prognosis for those with DIC, regardless of cause, is often grim: Between 20% and 50% of patients will die.
Herein, how serious is DIC?
Disseminated intravascular coagulation (DIC) is a rare but serious condition that causes abnormal blood clotting throughout the body's blood vessels. DIC may develop quickly over hours or days, or more slowly. Signs and symptoms may include bleeding, bruising, low blood pressure, shortness of breath, or confusion.
How does DIC happen?
Disseminated Intravascular Coagulation (DIC) Disseminated intravascular coagulation is a condition in which small blood clots develop throughout the bloodstream, blocking small blood vessels. The increased clotting depletes the platelets and clotting factors needed to control bleeding, causing excessive bleeding.
What is the most common cause of DIC?
Cancer
Who is at risk for DIC?
People who have one or more of the following conditions are most likely to develop DIC: Sepsis (an infection in the bloodstream) Surgery and trauma. Cancer.What do you give for DIC?
Treatment includes correction of the cause and replacement of platelets, coagulation factors (in fresh frozen plasma), and fibrinogen (in cryoprecipitate) to control severe bleeding. Heparin is used as therapy (or prophylaxis) in patients with slowly evolving DIC who have (or are at risk of) venous thromboembolism.What bacteria causes DIC?
DIC is classically associated with Gram negative bacterial infections but it can occur with a similar incidence in Gram positive sepsis. Moreover, systemic infections with other micro-organisms, such as viruses, Rickettsiae and even parasites (e.g. Plasmodium falciparum) may also result in DIC.How do you test for DIC?
In clinical practice, a diagnosis of DIC can often be made by a combination of the following tests : - Platelet count.
- Global clotting times (aPTT and PT)
- One or two clotting factors and inhibitors (eg, antithrombin)
- Assay for D-dimer or FDPs.
Is DIC hereditary?
The most common hereditary disorder causing excessive bleeding is Hemophilia A. Disseminated intravascular coagulation or DIC occurs as a result of obstetric complications such as abruptio placenta, saline abortion, retained products of conception, amniotic fluid embolism or severe pre-eclampsia/eclampsia.How does cancer cause DIC?
In DIC, the body is making many inappropriate clots throughout the body. Cancer can trigger DIC, particularly certain types of leukemia. DIC can also be related to sepsis (blood stream infection). DIC is considered an "oncologic emergency", which is an acute health problem caused by the cancer itself or its treatment.What is DIC in labor and delivery?
Disseminated intravascular coagulation (DIC) is a pathologic disruption of the finely balanced process of hemostasis. Even in the setting of fetal demise, labor and vaginal delivery of a pregnant woman with DIC carries the potential for catastrophic hemorrhage.What lab values indicate DIC?
Laboratory findings suggestive of DIC consist of a low platelet count, elevation of the D-dimer and fibrinogen concentrations, and prolongation of prothrombin time (PT) and activated partial thromboplastin time (aPTT).Is fibrinogen high or low in DIC?
However, because fibrinogen is an acute phase reactant, it can be elevated in patients with DIC associated with a chronic inflammatory disorder. A fibrinogen level of 300 mg/dl, while normal, may be lower than normal in a patient with a baseline high fibrinogen due to chronic inflammation.Can DIC cause pulmonary embolism?
Massive pulmonary embolism leading to cardiac arrest is associated with consumptive coagulopathy presenting as disseminated intravascular coagulation. DIC is not a disease or a symptom but a syndrome, which is always secondary to an underlying disorder.What does DIC stand for in cars?
Driver Information Center
What causes DIC in trauma?
Trauma-induced coagulopathy is coagulopathy caused by the trauma itself. The pathophysiology of trauma-induced coagulopathy consists of coagulation activation, hyperfibrino(geno)lysis, and consumption coagulopathy. These pathophysiological mechanisms are the characteristics to DIC with the fibrinolytic phenotype.What is acute DIC?
Acute DIC develops when sudden exposure of blood to procoagulants (eg, tissue factor [TF], or tissue thromboplastin) generates intravascular coagulation. In contrast, chronic DIC reflects a compensated state that develops when blood is continuously or intermittently exposed to small amounts of TF.What is the first sign of sepsis?
Sepsis Symptoms The first signs may include rapid breathing and confusion. Other common warning signs include: Fever and chills. Very low body temperature.What is it called when you bleed from every orifice?
What is Marburg? This Virus Causes Victims to Bleed From Every Orifice and Die. First recognized in 1967, Marburg virus, formerly known as Marburg haemorrhagic fever, is a rare but extremely fatal hemorrhagic disease.What does DIC mean in veterinary medicine?
Lee, DVM, DACVECC. Disseminated intravascular coagulation, commonly called DIC, is a common complication seen in emergency room (ER) or intensive care unit (ICU) pets.