Refeeding is the process of reintroducing food after malnourishment or starvation. Refeeding syndrome is a serious and potentially fatal condition that can occur during refeeding. It's caused by sudden shifts in the electrolytes that help your body metabolize food.Also, what causes refeeding syndrome?
The underlying causative factor of refeeding syndrome is the metabolic and hormonal changes caused by rapid refeeding, whether enteral or parenteral. On refeeding, the absorbed glucose leads to increased blood glucose levels, which increase insulin and decrease glucagon secretion.
One may also ask, which electrolyte abnormalities are seen in refeeding syndrome? The hallmark biochemical feature of refeeding syndrome is hypophosphataemia. However, the syndrome is complex and may also feature abnormal sodium and fluid balance; changes in glucose, protein, and fat metabolism; thiamine deficiency; hypokalaemia; and hypomagnesaemia.
Keeping this in view, how do you fix refeeding syndrome?
People with refeeding syndrome need to regain normal levels of electrolytes. Doctors can achieve this by replacing electrolytes, usually intravenously. Replacing vitamins, such as thiamine, can also help to treat certain symptoms. A person will need continued vitamin and electrolyte replacement until levels stabilize.
Is refeeding syndrome rare?
The refeeding syndrome is a rare, survivable phenomena that can occur despite identification of risk and hypocaloric nutritional treatment. Intravenous glucose infusion prior to artificial nutrition support can precipitate the refeeding syndrome. Starvation is the most reliable predictor for onset of the syndrome.
How do you prevent refeeding syndrome?
“the risk of refeeding syndrome should be avoided through gradual increase of caloric intake and close monitoring of weight, vital signs, fluid shifts and serum electrolytes”. It, however, did not advise on how many calories to start, by how many calories to increase, nor how often to increase calories.What does refeeding syndrome feel like?
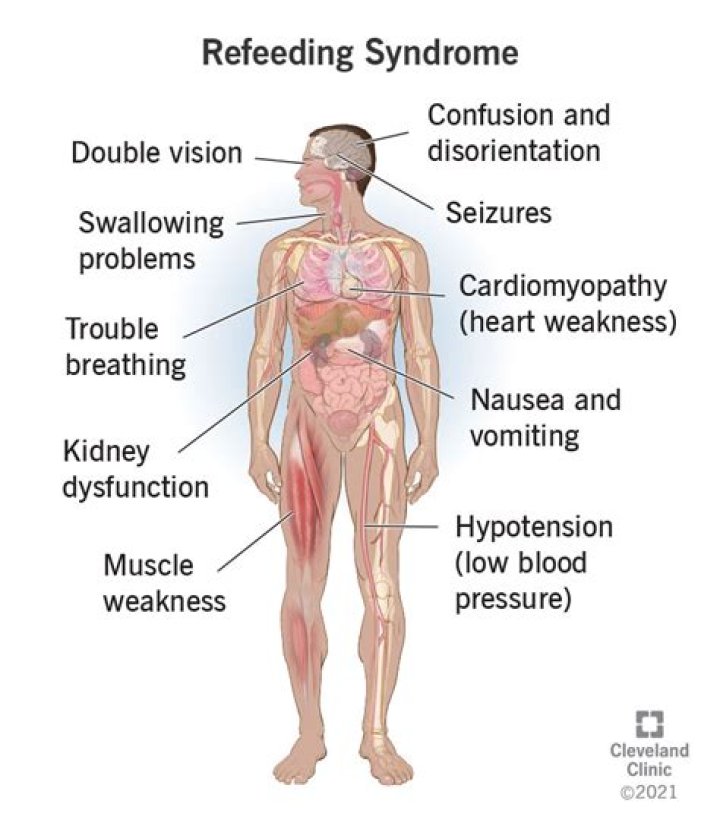
Symptoms of refeeding syndrome may include: fatigue. weakness. confusion.How long does it take to develop refeeding syndrome?
Refeeding syndrome usually occurs within four days of starting to re-feed.How do you know if you have refeeding syndrome?
Monitor for neurologic signs and symptoms. Your patient with refeeding syndrome may develop muscle weakness, tremors, paresthesias, and seizures. Institute seizure precautions. In addition, she may have cognitive changes, including irritability and confusion.How do you treat refeeding syndrome?
People with refeeding syndrome need to regain normal levels of electrolytes. Doctors can achieve this by replacing electrolytes, usually intravenously. Replacing vitamins, such as thiamine, can also help to treat certain symptoms. A person will need continued vitamin and electrolyte replacement until levels stabilize.What should you eat if you are malnourished?
You need to eat a variety of foods from the main food groups, including: - plenty of fruit and vegetables.
- plenty of bread, rice, potatoes, pasta and other starchy foods.
- some milk and dairy foods.
- some meat, fish, eggs, beans and other non-dairy sources of protein.
Can you survive on TPN?
The long-term survival prospects of patients maintained through total parenteral nutrition vary, depending on the cause of intestinal failure. Three-year survival of TPN-dependent patients ranges from 65 to 80 percent.How much thiamine should I take for refeeding syndrome?
Prevention and treatment Also 50 to 250 mg of thiamine should be given especially when glucose is infused. More thiamine may be necessary until the patient is stabilized. The energy intake should start at a maximum of 50% of planned energy intake (500–1000 kcal dayÀ1).What happens if you eat a lot after starving?
Eating again after a period of starvation Let's say you're in a position where you have no access to food for a few weeks, but then the situation suddenly changes. Having too little phosphate in the blood can cause delirium, muscle weakness, or even cardiac arrest when food is reintroduced.How do you refeed after drying fast?
Treat your body gently when you are dry fasting. Engage in activities that calm your senses like yoga, meditation etc. Avoid being in the sunlight or any environment that drains your energy. Try journaling your journey whenever you feel demotivated.How do you eat after starving?
Resuming eating after starvation will require a doctor's supervision and may involve eating boiled vegetables, lactose-free foods, and a low-protein, low-sugar diet.Does fasting deplete magnesium?
Electrolytes – essential minerals such as potassium, calcium, sodium, and magnesium – play crucial roles in cellular function. Fasting can deplete the body's stores of electrolytes, especially during prolonged fasts or during periods of exercise when electrolytes can be lost during sweat.How do you refeed after 48 hours fast?
Summary A 48-hour fast involves abstaining from eating for 2 consecutive days, usually done once or twice per month. It's important to drink plenty of fluids during the fast and slowly reintroduce food afterward. Take a quick survey.How long does it take for an anorexic to gain weight?
Most people with severe AN need to consume an additional 1,000+ calories per day to gain just one pound per week. If someone with AN needs to gain over thirty pounds, weight restoration can take many months. On a daily basis, the hardest part for many people is eating every two to three hours.What do you monitor for refeeding syndrome?
A tachycardia has been reported to be a useful sign in detecting cardiac stress in the refeeding syndrome. Plasma electrolytes, in particular sodium, potassium, phos- phate, and magnesium, should be monitored before and during refeeding, as should plasma glucose and urinary electrolytes.Why are alcoholics at risk for refeeding syndrome?
There are several risk factors for developing re-feeding syndrome including: unintentional weight loss, low nutrient intake for more than 7 days, AN, chronic alcoholism, depression in the elderly, patients with cancer, chronic infectious diseases, homelessness, and social deprivation [4].Can fasting cause low potassium?
Prolonged fasting or cleanses and extremely limited food intake after bariatric surgery may also lead to low potassium. Too little potassium may lead to elevated blood pressure, kidney stones, and/or bone loss. Conversely, obtaining enough potassium in the diet may reduce the risk and severity of these conditions.