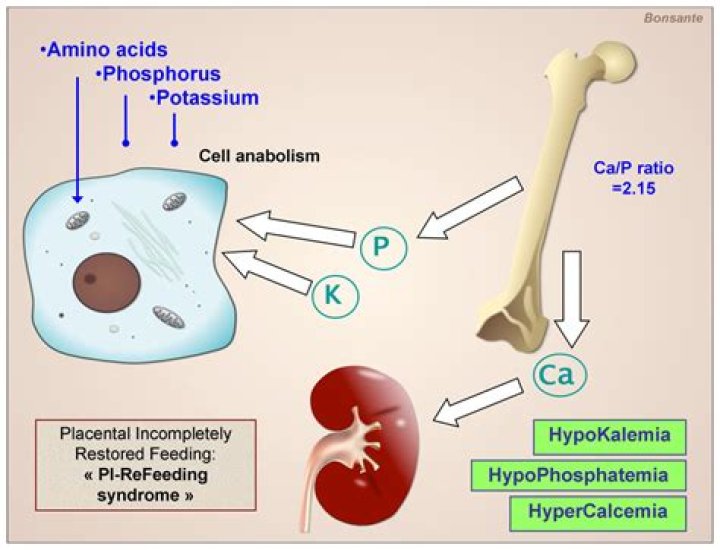
Consequently, how does refeeding syndrome occur?
Refeeding syndrome can develop when someone who is malnourished begins to eat again. The syndrome occurs because of the reintroduction of glucose, or sugar. As the body digests and metabolizes food again, this can cause sudden shifts in the balance of electrolytes and fluids.
Also Know, how do you prevent refeeding syndrome? Measure serum electrolyte levels and correct abnormalities before refeeding, as low levels of potassium, magnesium, and phosphate may be a risk factor for refeeding syndrome. Obtain serum chemistry values every 3 days for the first 7 days and then weekly during the rest of the refeeding period.
Similarly, how do you know if you have refeeding syndrome?
Monitor for neurologic signs and symptoms. Your patient with refeeding syndrome may develop muscle weakness, tremors, paresthesias, and seizures. Institute seizure precautions. In addition, she may have cognitive changes, including irritability and confusion.
How long does it take to develop refeeding syndrome?
Refeeding syndrome usually occurs within four days of starting to re-feed.
What does refeeding syndrome feel like?
Symptoms of refeeding syndrome may include: fatigue. weakness. confusion.How long can you not eat before refeeding syndrome?
Any patient with negligible food intake for more than five days is at risk of developing refeeding problems.How much thiamine should I take for refeeding syndrome?
Prevention and treatment Also 50 to 250 mg of thiamine should be given especially when glucose is infused. More thiamine may be necessary until the patient is stabilized. The energy intake should start at a maximum of 50% of planned energy intake (500–1000 kcal dayÀ1).What happens if you feed a starving person?
Refeeding syndrome is a potentially fatal clinical condition characterized by severe electrolyte and fluid shifts associated with metabolic abnormalities in severely malnourished or starved patients undergoing oral, enteral or parenteral refeeding.Why are alcoholics at risk for refeeding syndrome?
There are several risk factors for developing re-feeding syndrome including: unintentional weight loss, low nutrient intake for more than 7 days, AN, chronic alcoholism, depression in the elderly, patients with cancer, chronic infectious diseases, homelessness, and social deprivation [4].How do you refeed after fasting?
Some of the best foods to have immediately after breaking a fast include:- Freshly-made fruit and vegetable juices.
- Raw fruits.
- Bone broths.
- Fermented foods, such as yogurt (opt for unsweetened), kefir, sauerkraut, etc.
- Leafy green lettuces, sun as spinach, kale, etc.
How do you treat refeeding syndrome?
People with refeeding syndrome need to regain normal levels of electrolytes. Doctors can achieve this by replacing electrolytes, usually intravenously. Replacing vitamins, such as thiamine, can also help to treat certain symptoms. A person will need continued vitamin and electrolyte replacement until levels stabilize.How do I recover from weight gain?
What to do if you are coping with weight gain in recovery- See a trained treatment team.
- Follow your meal plan.
- Acceptance is a crucial step in recovery.
- Develop a support network.
- Donate old clothes.
- Remind yourself why you chose recovery.
How do you monitor for refeeding syndrome?
Serum electrolytes should be checked after 8 – 12 hours of nutrition support initially, then daily during the refeeding period (first 48-72 hours). The frequency and duration of electrolyte monitoring will vary depending on the degree of malnutrition and whether electrolyte disorders occur, as well as their severity.Is refeeding syndrome rare?
The refeeding syndrome is a rare, survivable phenomena that can occur despite identification of risk and hypocaloric nutritional treatment. Intravenous glucose infusion prior to artificial nutrition support can precipitate the refeeding syndrome. Starvation is the most reliable predictor for onset of the syndrome.Can fasting cause low potassium?
Prolonged fasting or cleanses and extremely limited food intake after bariatric surgery may also lead to low potassium. Too little potassium may lead to elevated blood pressure, kidney stones, and/or bone loss. Conversely, obtaining enough potassium in the diet may reduce the risk and severity of these conditions.What are the symptoms of low phosphate?
Symptoms of hypophosphatemia occur only when the phosphate level in blood becomes very low. Muscle weakness develops, followed by stupor, coma, and death. In mild chronic hypophosphatemia, the bones can weaken, resulting in bone pain and fractures. People may become weak and lose their appetite.How do you fix low phosphate?
Therefore, your healthcare provider may suggest magnesium or Vitamin D supplements, if your phosphorous is low. You may also be ordered a medication to lower your blood calcium levels, if it is elevated. Phosphate supplementation - Can be either intravenous (IV) with extremely low levels, or it can be by mouth.How do you get electrolytes?
Electrolytes are minerals that carry an electrical charge. They're vital for health and survival. Electrolytes spark cell function throughout the body.Foods with electrolytes include:
- spinach.
- kale.
- avocados.
- broccoli.
- potatoes.
- beans.
- almonds.
- peanuts.
What is refeeding syndrome in anorexia?
Refeeding syndrome occurs when patients that have been starved begin to eat and metabolize calories. The body shifts from a catabolic state (a state of breaking down tissues for nutrients) to an anabolic state (a state of rebuilding tissues/growth).What does Hypophosphatemia mean?
Hypophosphatemia is an electrolyte disorder in which there is a low level of phosphate in the blood. Symptoms may include weakness, trouble breathing, and loss of appetite.How do you help a starving dog?
7 Tips for Caring for a Malnourished Dog – Environment, Food and Probiotics- Provide a warm, comfortable, safe environment.
- Breakfast!
- Snacks are the key.
- High-protein lunch and dinner.
- Give something to munch on.
- Give a probiotic supplement.
- Regular vet visits.