Then, what does renin do in the kidneys?
Renin's primary function is therefore to eventually cause an increase in blood pressure, leading to restoration of perfusion pressure in the kidneys. Renin is secreted from juxtaglomerular kidney cells, which sense changes in renal perfusion pressure, via stretch receptors in the vascular walls.
Also, how do kidneys affect blood pressure? If the kidneys' blood vessels are damaged, they may stop removing wastes and extra fluid from the body. Extra fluid in the blood vessels may then raise blood pressure even more, creating a dangerous cycle.
Moreover, how does renin affect urine production?
ANP promotes natriurisis by shutting down the renin-angiotensin-aldosterone system and causing vasodilation. As the blood vessels expand, urine excretion of sodium and water increases, stabilizing blood volume and blood pressure.
What would happen to your blood pressure if your kidneys could not regulate the production of renin?
Without renin, blood pressure cannot be protected in the face of sodium depletion. Conversely, in the face of salt loss, excess renin production serves only to maintain, not to increase blood pressure. It is in salt-replete humans that renin may be undesirable and contribute both to hypertension and end-organ damage.
What is renin in the body?
Renin. enzyme. Renin, enzyme secreted by the kidney (and also, possibly, by the placenta) that is part of a physiological system that regulates blood pressure. In the blood, renin acts on a protein known as angiotensinogen, resulting in the release of angiotensin I.How does renin affect blood pressure?
Renin by itself does not really affect blood pressure. Instead, it floats around and converts inactive forms of angiotensin into angiotensin I. These inactive forms of angiotensin, which are produced by the liver, are not able to alter the blood pressure until renin changes them into angiotensin I.Which organ produces renin and erythropoietin?
kidneysWhere is Chymosin found?
Rennin, also called chymosin, protein-digesting enzyme that curdles milk by transforming caseinogen into insoluble casein; it is found only in the fourth stomach of cud-chewing animals, such as cows. Its action extends the period in which milk is retained in the stomach of the young animal.What causes an increase in renin?
Patients with secondary hyperaldosteronism (that is, caused by kidney disease or renal vascular disease) will have increased plasma levels of renin and aldosterone. Renin is an enzyme released by specialized cells of the kidney into the blood. It is in response to sodium depletion or low blood volume.What cells release renin?
juxtaglomerular cellsWhat is the normal range for renin?
Normal Results For low sodium diet, normal value range is 2.9 to 24 ng/mL/hour (2.9 to 24 µg/L/hour). Normal value ranges may vary slightly among different laboratories. Some labs use different measurements or test different samples. Talk to your doctor about the meaning of your specific test results.Is renin a vasodilator?
Cardiorenal Effects of Renin Inhibitors Dilate arteries and veins by blocking angiotensin II formation. This vasodilation reduces arterial pressure, preload and afterload on the heart.What hormone increases urine output?
Antidiuretic hormoneWhy are my kidneys producing too much urine?
Diabetes mellitus (often simply called diabetes) is one of the most common causes of polyuria. In this condition, high amounts of glucose (blood sugar) collect in your kidney tubules and cause your urine volume to increase. It can also increase if your kidneys can't properly control the fluid passing through them.What does high renin mean?
A high level of renin may be due to: Adrenal glands that do not make enough hormones (Addison disease or other adrenal gland insufficiency) High blood pressure caused by narrowing of the kidney arteries (renovascular hypertension) Liver scarring and poor liver function (cirrhosis) Loss of body fluid (dehydration)What hormone does kidney produce?
Hormone secretion The kidneys secrete a variety of hormones, including erythropoietin, calcitriol, and renin. Erythropoietin is released in response to hypoxia (low levels of oxygen at tissue level) in the renal circulation. It stimulates erythropoiesis (production of red blood cells) in the bone marrow.Can hormones affect kidney function?
A high level of a hormone is associated with an increased risk of kidney failure and death among patients with chronic kidney disease (CKD). The discovery could lead to earlier diagnosis and treatment of patients at risk. CKD affects an estimated 23 million American adults.What regulates salt in the body?
Aldosterone. Aldosterone is a steroid hormone. Its main role is to regulate salt and water in the body, thus having an effect on blood pressure.What causes urine to flow from the kidneys to the bladder?
From the kidneys, urine travels down two thin tubes called ureters to the bladder. The ureters are about 8 to 10 inches long. Muscles in the ureter walls constantly tighten and relax to force urine downward away from the kidneys. If urine is allowed to stand still, or back up, a kidney infection can develop.Does the urinary system regulate blood glucose levels?
The role of the excretory system is to remove waste products such as urea, uric acid, and creatinine from the blood to be passed out of the body as urine. The urinary system also helps us to regulate the amount of glucose, salts and water in the blood.Which organs are involved in the renin angiotensin aldosterone system?
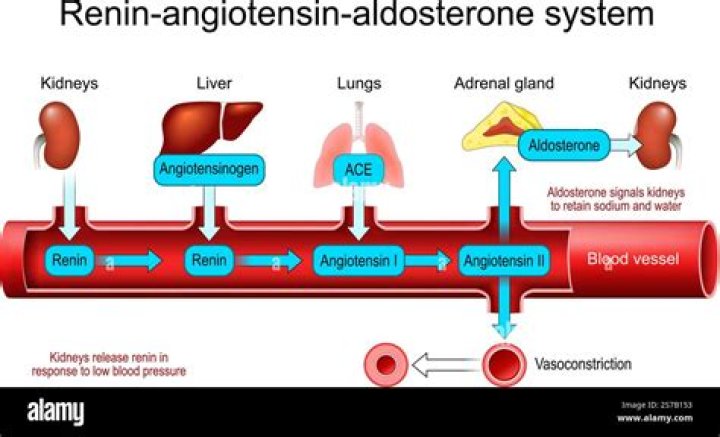
Fountain JH, Lappin SL.- Introduction. The renin–angiotensin–aldosterone system (RAAS) is a critical regulator of blood volume and systemic vascular resistance.
- Organ Systems Involved. The RAAS involves the kidneys, lungs, systemic vasculature, and the brain.
- Function.
- Mechanism.
- Clinical Significance.
- Questions.